Surgery for Thoracic Outlet Syndrome – Is It Worth It?
Functional training may help relieve thoracic outlet syndrome symptoms, including cold and numb hands. Learn the risks of TOS surgery, along with less-risky thoracic outlet syndrome treatments, including simple movement solutions that address muscle dysfunction.
Table of Contents
What is Thoracic Outlet Syndrome?
Should You Get Surgery for Thoracic Outlet Syndrome?
What are the Complication Rates with Thoracic Outlet Surgery?
What are the Success Rates of Thoracic Outlet Syndrome?
What will my Quality of Life be Post Thoracic Outlet Syndrome Surgery?
What are the Alternatives to Thoracic Outlet Syndrome Surgery?
How I Fixed my Thoracic Outlet Syndrome Symptoms
Functional Training Exercises for Relieving Symptoms of Thoracic Outlet Syndrome
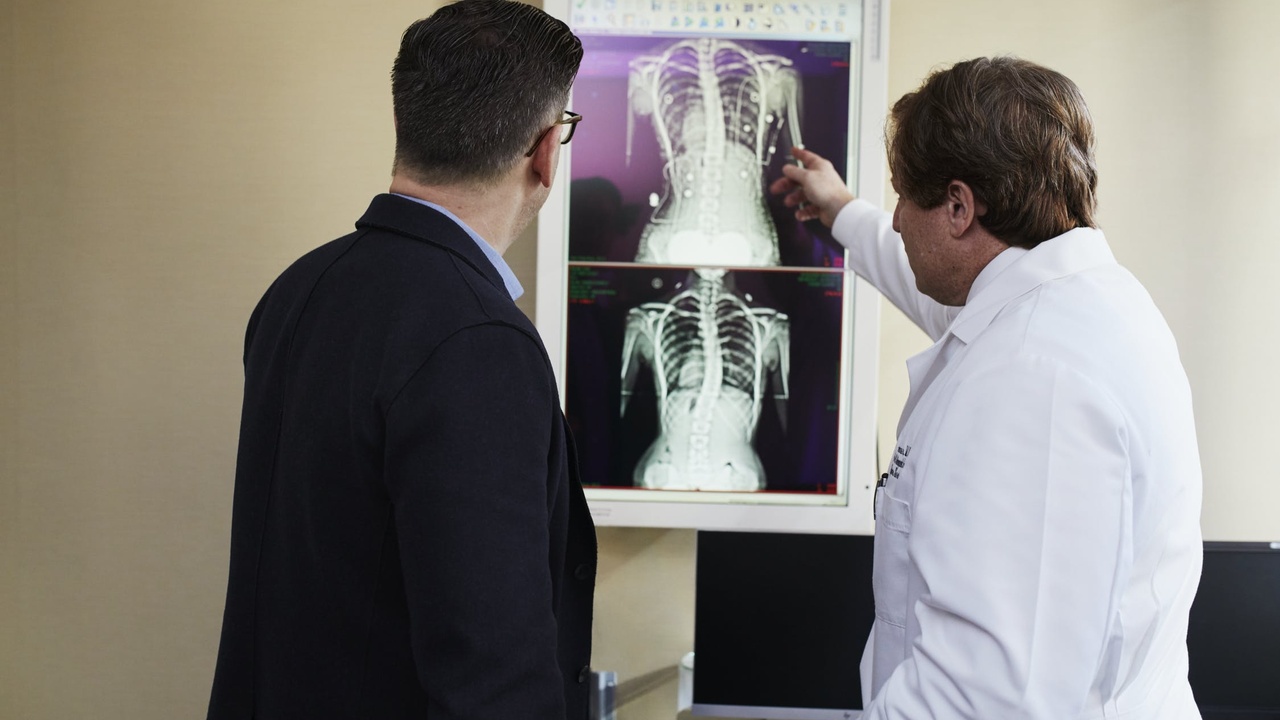 Does your spine look similar?
Does your spine look similar?
If you're reading this you may have been told you have Thoracic Outlet Syndrome (TOS).
If you’ve seen any of my videos on thoracic outlet syndrome, you know that I was diagnosed with this syndrome as a teenager and had some pretty troubling symptoms in my shoulders, hands, and wrists from the ages of 19 to 22. The veins in my arms disappeared. I experienced constant numbness, coldness, tingling, and aching. Typing for just five minutes was a sure-fire way to cause more pain.
The doctors I saw insisted that my symptoms were the result of overuse; that I had an overuse injury. They prescribed rest.
But the problems didn’t heal on their own.
I struggled for years, trying everything from massage and chiropractic work to taking vitamin B.
Eventually, I figured out how to gradually retrain my muscles to get my shoulders back in the right place. It took a few months to get to where I was generally comfortable on a daily basis. It took me a few years of trial and error to figure out how to get even more strong, stable, and resilient after that.
I'm happy to report that now I can do cartwheels and type on the computer without issue or symptoms.
You may be experiencing your own numb, cold, and tingling hands, or shoulder and neck pain, and someone has told you that you have a bone impingement, or a labral or rotator cuff tear, or TOS, and that surgery is the only way to make these symptoms go away.
In this post, we're going to dive deep into the research on the diagnosis of TOS and the real results of surgery. We'll also talk about what you can do to help yourself without going under the knife.
What is Thoracic Outlet Syndrome?
Thoracic outlet syndrome is complex. There is confusion regarding its diagnosis, treatment, prognosis, and even what to call it. As Jordan Gliedt, DC, stated in his 2013 research, published in the journal Topics in Integrative Health Care, “Thoracic outlet syndrome remains a challenging, controversial, and often misunderstood and misdiagnosed upper extremity disorder.”
TOS is characterized by the compression of nerves, veins, and arteries that travel from your neck to your arms and hands. Often the compression is caused by your first, or top, rib, and so the surgical solution is to remove that rib.
But posture plays a critical role, too. The symptoms get worse when you’re hunched over a computer all day, for example (we used to call TOS, typist syndrome).
Should You Get Surgery for Thoracic Outlet Syndrome?
While some traditional treatment protocols try to release tight muscles first, when that doesn’t work, they jump right into surgery recommendations.
Many researchers will tell you that surgery is not a sure or easy fix, going so far as to say that thoracic outlet syndrome surgical procedures should be reserved for rare patients with documented worsening of neurologic function.
Based on my experience, identifying and treating muscle dysfunction and imbalance is just as, if not more, effective than surgery.
An important issue to reflect on is whether your doctor is looking at you from a surgical perspective or a holistic perspective. One study showed that surgeons diagnose TOS 100 times more frequently than neurologists.
Let's examine what the research shows on treatment through invasive surgery, and attempt to make this complex information a little more simple. There are several research studies that demonstrate good outcomes with surgery, but, as you will see, they are not without flaws.
What are the Complication Rates with Thoracic Outlet Surgery?
I’ll start out by saying that there are no reports of death or anything extremely severe happening in any large numbers, so the risks of truly bad complications of TOS surgery appear to be limited.
In a 2017 study of 102 TOS surgeries, researchers evaluated complications over a two-year period after the procedures. Nearly 45 percent of patients experienced problems ranging from pneumothoraxes (an abnormal collection of air in the space around the lungs, which can cause difficulty breathing and is typically treated with a chest tube or needle aspiration) to vein and nerve injury.
Another study, from 1995, boasted 81.4% of 118 patients had good to excellent results following surgical intervention. In this study, good is defined as mild residual symptoms, and a return to work and some sports. Of this group, 34.3% of patients had minor complications following surgery. A second surgery had to be completed in 13.5% of patients.
All in all, the complications don't seem to be too bad. So let’s consider how effective or successful surgery is for thoracic outlet syndrome.
 Make typing fun again. Credit: Norwood Themes on Unsplash
Make typing fun again. Credit: Norwood Themes on Unsplash
What are the Success Rates of Thoracic Outlet Syndrome?
In 2004, a study published in the Annals of Vascular Surgery examined the outcome of 176 thoracic outlet syndrome surgeries at the two-year mark, via a phone survey. Nearly half (49.4 percent) of patients said they were excellent, 34.6 percent said they were good, 8 percent of patients said they were fair, and 8 percent said they were poor.
It sounds promising, since 84 percent of patients had good or excellent results at the two-year mark, right? In the classification used for this study, “good” is defined as having intermittent pain that is well-tolerated, and a possible return to professional and leisure activities. So, even with “good” results, some patients weren’t back to work or fun.
While good sounds good, sometimes it may actually mean a life still plagued by pain.
And while researchers may report, on the surface, that outcomes are “good” and surgery is successful, a vast majority of the time, longer-term results don’t tell the same story.
In a 2001 study, published in the World Journal of Surgery, researchers examined patients post TOS surgery. Of the 23 patients who had surgery, only 2 had complications. Nineteen out of the 23 reported full relief, while the remaining four reported only partial relief of their symptoms. These results sound pretty promising, until you look more closely at the length of the follow-up period.
Patient responses were recorded within three months to a year post operatively. That may not seem significant, but it is. A short follow-up period means you really don’t know if the treatment worked. After three months, patients may not have even gone back to “normal life” to truly test the result of the surgery. Even within a year, they may not have had enough time to put things to the test.
The danger of this short follow-up period is that symptoms can and do come back within years after the surgery. Without longer-term follow up, it’s actually impossible to say surgery was successful.
A great example of this is a 2018 study on the long-term surgical outcomes of 56 TOS patients. Ninety percent of them reported improvements in symptoms and 54 percent of them reported complete relief of symptoms 1 to 11 years out. (Long-term functional impairment remained higher than expected and higher than the general population.)
The long-term follow-up in this study, from 1 to 11 years, is a large window in which a lot can happen.
Of the 41 study subjects who answered questionnaires about long-term results, it’s unclear how far out from surgery they were. Results from 1 year post-surgery could differ dramatically from 11 years out. It’s possible things went well for 11 years, but unlikely.
The recurrence of TOS symptoms most often occurs within the first two years following surgery: 60 percent of patients experience symptoms in the first year (along with persistent disability), while 80 percent experience a recurrence of symptoms in the second year, according to research published in Current Pain and Headache Reports in 2011.
Translation: within two years, the majority of patients have their symptoms come back.
 Life would be so simple if we didn’t have muscles. Credit: Nino Liverani.
Life would be so simple if we didn’t have muscles. Credit: Nino Liverani.
In another article, published in 2003 in the Annals of Thoracic Surgery, researchers reviewed 72 patients between 14 and 24 months post-surgery. The outcomes were measured in a follow-up clinic to assess for symptoms, complete range of motion, and return to previous activities without any restrictions. Complete resolution of symptoms occurred in 63.9 percent of patients, while 23.6 percent of patients experienced a partial recovery, and 9 percent reported no resolution.
You can find other studies with less impressive results, too. In one, only 21 percent of 409 patients who had TOS surgery felt complete relief, while 32 percent reported good relief, 25 reported they were doing fair, and 22 percent experienced no improvement.
Perhaps the most telling study results were published in 2001 in the Journal of Vascular Surgery. Researchers looked at both short- and long-term TOS surgery outcomes.
At approximately 10 months out, 80 percent of patients who responded (167 out of 238) reported improvements in pain, paresthesias, and range of motion. This demonstrated good positive results with pain and movement, but did that translate into function?
Only 50 percent of patients had returned to full activity, while 9 percent continued their use of narcotics and 20 percent were still using over-the-counter pain medications.
At 47 months out, 65 percent of those who responded (only 89) reported an improvement in symptoms, and 64 percent reported satisfaction, while 35 percent remained on medication, and 18 percent were disabled.
One big concern with this study, as the authors noted, is what happened to those who did not return their questionnaires. Did they have more depression, more disability, more pain, and less motivation to communicate? While the shorter-term results were positive, the long-term results are not as clear.
Also, reports of “satisfaction” can skew results to look good. Patients were relatively satisfied with surgery results, but they may not have explored other options that may have been less invasive and more effective. Would they have been more satisfied if they had successfully treated symptoms with targeted functional training instead of surgery?
In 2010, a study published in the British Journal of Neurosurgery, compared a group of patients who received operations to a group of patients who received conservative treatments. These groups were also matched to a healthy control group for further comparison. The researchers were looking at several outcomes, including quality of life, function, and pain.
Unsurprisingly, patients with TOS have decreased quality of life compared to their healthy counterparts regardless of their treatments. Of the patients who had surgery, 15 out of 18 would choose to have surgery again, but 4 of those 15 did not feel like the first surgery reduced their symptoms!
In looking at function, the researchers found that there was no difference in the limitations of the group that had surgery versus the group who received conservative treatment.
As you can see, while many studies report success, if you dig deeper into the literature, you begin to notice inconsistencies. A successful surgery may indicate that it was complication-free, initially, but that does not equal successful results for what a patient is looking for in the longer-term -- including are turn to work, being off pain medication, and leaving thoracic outlet syndrome in the past. Much of the peer-reviewed literature about TOS surgery results can be misleading, whether it is about short-term or long-term results.
See also: Do Injections for Pain Work?
What will my Quality of Life be Post Thoracic Outlet Syndrome Surgery?
In the British Journal of Neurosurgery study, researchers wrote that if the goal of surgery is to improve quality of life, they felt “the benefit of decompressive surgery was found to be questionable.”
Another study published in the Journal of Vascular Surgery looked more specifically at the return to work following TOS. Researchers followed-up with 79 patients with an average of 4.2 years from the initial intervention—either surgical or more conservative. Of this group, 19 percent had surgical interventions, and 81 percent tried conservative solutions.
Researchers found that surgical patients had more missed work time than those who were treated without surgery. The overall return to work, after nearly 4 years, was 78 percent in the nonsurgical group and only 60 percent in the surgical group.
Regardless of surgical or nonsurgical treatment, the symptoms and pain were similar in each group. This again reiterates that surgery does not mean you will be pain- or symptom-free after surgery, even after over four years.
In one case, a patient wrote up her story of how disappointing surgery can be. She had seven total surgeries over the years of her treatment and remained on pain medication for daily pain relief. She still relied on family and friends to help her with daily activities.
See also: Why you DON’T Need Orthopedic Surgery for Joint Pain
What are the Alternatives to Thoracic Outlet Syndrome Surgery?
It’s pretty clear that all patients with thoracic outlet syndrome should start with something noninvasive to address the musculoskeletal components of these issues.
Here is a recent student of mine who successfully fixed his thoracic outlet syndrome with functional movement training:
Kyle shares his experience avoiding thoracic outlet syndrome surgery.
Turning to surgery, cutting muscles, and removing bones is going to have consequences for how you move. Other muscles will have to coordinate motion and learn functions they weren’t originally designed to do. I talk about how to avoid some of those consequences here.
But essentially, you can think of your TOS as a rock (the bones) blocking the flow of a hose (your veins and nerves). You can use functional training to get your muscles to move that rock so it’s no longer obstructing blood flow!
There’s evidence that exercise can help with thoracic outlet syndrome. A 1997 study reviewed non-operative treatment research. Researchers found that patients who started with intensive inpatient rehabilitation and continued with home exercises had 88 percent subjective improvement, and 73 percent returned to work. The follow-up was an average of two years after initiation, which, as discussed earlier, is a more appropriate length for follow-up results.
While many people who have been diagnosed with TOS may have tried physical therapy and rehabilitation, it’s important to recognize that not all protocols for thoracic outlet syndrome are effective for everyone. If you do the wrong exercises, you’ll see little to no improvement.
You’ll notice that many conventional protocols for thoracic outlet syndrome focus on stretching and relaxing muscles around the neck and shoulder. This will not help if weak muscles are unable to achieve and maintain good postural position. Massaging your neck and shoulders is NOT a long term solution for muscle dysfunction.
Some physical therapy protocols do the right thing, but poor coaching and attention to detail from a physical therapist (or aide) and no long-term plan for strength and stability will undermine any hope of resolution (like this one from UHN.ca).
See also: How to Fix Chronically "Tight" Muscles
Probably the most crucial thing to do when looking at solving your thoracic outlet syndrome problems is examine your own goals and expectations.
- Do you need to return back to work?
- How quickly?
- Does your work include physically demanding or repetitive tasks?
- Are you planning on returning back to recreational activities?
- Are you hoping to be completely pain free?
- Would you like to be off of all pain medications?
- Do you realize you still may need other treatments after surgery (like physical therapy, injections, potential repeat surgeries)?
- If you tried conservative treatment, did you feel that the regimen you were on was actually targeting the right things?
- If you felt like things were going the right way, did you push through at a consistent pace to make progress? If not, doubling down on your efforts may be very helpful.
- If you felt like the guidance you were getting wasn’t helping, have you tried finding help elsewhere?
Finding someone who understands how to train your body to move and feel better can be difficult, but it’s a crucial piece of the puzzle. Once you understand how to train your body properly, you have a much better chance of solving your problems for the long term in a non-invasive, non-surgical way.
See also: How to Identify Muscle Dysfunction and Imbalance
How I Fixed my Thoracic Outlet Syndrome Symptoms
When my symptoms were at their worst, typing for even a few minutes would cause my hands, wrists, and elbows to throb. My arms would feel cold and numb.
When I was walking around farmers markets with my then-girlfriend (now wife), I remember feeling my hands and forearms aching from doing absolutely nothing. I would constantly pull at my sweater sleeves thinking that tight sleeves were causing my discomfort!
Now, I’m able to type out long articles like this without experiencing pain. I can sleep through the night without forearm pain. And I can’t remember the last time I pulled at my sweater sleeves to “fix” my numb hands! 😅
So how did I improve my thoracic outlet symptoms?
I addressed the muscle dysfunction and imbalance that was affecting my posture (i.e. bone position).
One of the most important things you can do to improve your thoracic outlet symptoms is to open up the muscles of your chest and anterior shoulders.
Functional Training Exercises for Relieving Symptoms of Thoracic Outlet Syndrome
Some simple stretching and strengthening exercises for your chest and shoulders will often yield big improvements for hand and wrist pain from TOS.
Here’s one that you can try easily at home. Make sure you use the contractions as mentioned in the video to get the most bang for the buck!
Chest stretch to improve blood flow through the thoracic outlet.
Now that you’ve opened your chest and shoulders, you want to build some strength in the shoulder muscles to stabilize the improved position.
Try this shoulder exercise for 20-60 seconds in each direction. Go as high as you can go without your hands going alarmingly numb. Each time you do this exercise, see if you can get just a tiny bit higher. The goal is to gradually teach your body to control a bigger and bigger range of motion. Tiny changes add up over time!
Exercise to improve shoulder strength and position to reduce TOS symptoms
You can do these exercises throughout the day, several times a day.
Since modern life often has us trapped in closed-off, lazy shoulder positions, taking stretch breaks for these exercises will add a healthy amount of movement.
When you first start, know that some muscle soreness may occur and is totally normal. Just take your time to acclimate and keep your intensity low for a week or two. Over time, you can do more sets and reps as your body gets used to the movements.
If you’ve got thoracic outlet symptoms, these two exercises alone may feel like a huge benefit immediately. For some people, it may take a little bit of time to feel the benefits of better shoulder positioning.
If you find that these exercises DON’T provide massive benefits for you right away, don’t fret.
For some people, addressing more muscles around the shoulders, neck, and spine will be necessary to get better bone positioning, and therefore better function neck, to shoulder, to fingertips.
Retraining your muscles to reduce symptoms of thoracic outlet syndrome can take time. It’ll require you to think outside the standard physical therapy protocols for thoracic outlet syndrome, but it’s well worth the time and effort.
I've put everything I learned over the years into a program called The Shoulder Fix that’s designed to help you help yourself. Check it out if you're looking for a straightforward way to help yourself at home.
If you want to start with the basics, read my article on How to Identify Muscle Dysfunction and Imbalance.
For a better understanding of pain, read How Shifting Your Perspective on Chronic Pain can Help You Heal.
For more functional training exercises that can help relieve the symptoms of thoracic outlet syndrome, check out The Shoulder Fix.

